Journal of Clinical Neuroscience and Rehabilitation
Alleviating Neurological Sleep Disorders through Targeted Rehabilitation using Restorative-Therapeutic Surfaces in New Zealand
Sleep Specialist, New Zealand
Author and article information
Cite this as
Satralkar M. Alleviating Neurological Sleep Disorders through Targeted Rehabilitation using Restorative-Therapeutic Surfaces in New Zealand. J Clin Neurosci Rehabil. 2026;2(1):027-031. Available from: 10.17352/jcnr.000005
Copyright License
© 2026 Satralkar M. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Abstract
Neurological sleep disorders such as insomnia, obstructive sleep apnea, narcolepsy, and restless legs syndrome are highly prevalent in New Zealand, imposing a considerable public health and quality-of-life burden. Adult insomnia alone affects approximately one in four adults, and its prevalence has risen over the past several decades. Complex interactions between sleep disorders, circadian rhythms, and sleep environment factors with a specific emphasis on bedding or sleeping surfaces are studied. Utilizing epidemiological data, advancements in material science as well as clinical research in sleep medicine, the paper initially delineates the circadian and neurological mechanisms underlying prevalent sleep disorders. It subsequently examines how sleep surface characteristics, including firmness calibration and ergonomic zoning for spinal alignment, temperature regulation, and allergen load, collectively influence sleep latency, sleep efficiency, and the continuity of sleep architecture. Condition-specific sections connect specialty bedding prescriptions with pathophysiology. For example, medium-firm seven zone hybrid mattresses can help with insomnia and chronic snoring can be reduced using an adjustable base to elevate upper body for obstructive sleep apnea, medium to soft surfaces for side-sleeping support reduces apnea events and for narcolepsy, pressure-relieving surfaces that accommodate multiple sleep positions support the irregular sleep-wake patterns characteristic of this disorder. Finally, for restless legs syndrome, cooler bedding temperatures can help reduce symptom severity, while mattresses supporting the lower back maintain proper spinal alignment to minimize discomfort. Overall, the findings support restorative-therapeutic surfaces as a practical, scalable adjunct to pharmacological and behavioral therapies, with the potential to reduce symptom burden, enhance rehabilitation outcomes, and inform consumer, clinical, and industry decision-making around sleep-health interventions in New Zealand.
Introduction
Defining sleep disorders
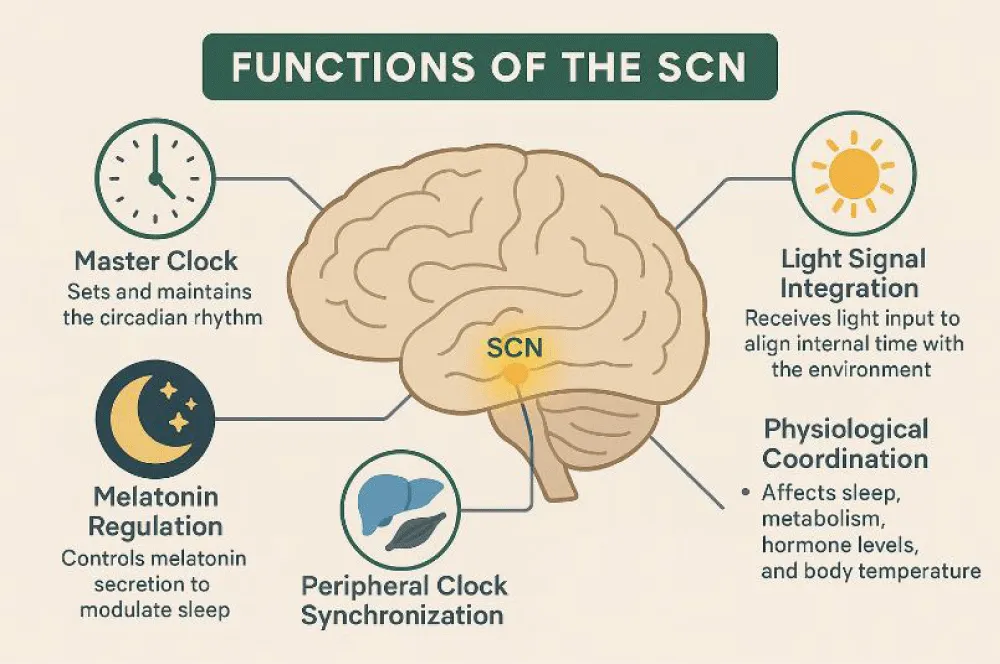
Circadian rhythms are natural rhythms of the human body which are periodic or repetitive over a 24-hour cycle [1]. These intrinsic rhythms include sleep-wake cycles, hormone secretion, body temperature, metabolic cycles, cardiovascular rhythm, cognitive performance, immune function, etc. The supra-chiasmatic nucleus (SCN) is the human body clock or biological clock. It acts as a ‘master pacemaker’ to synchronize intrinsic physiological rhythms by receiving inputs from external environmental cues known as ‘zeitgebers’ (or time givers) such as light-dark cycles, temperature, social cues, food, medication, exercise, etc. The major function of the SCN is to receive light input to align internal time with the external environment to control melatonin secretion thereby modulating sleep [2] as seen in Figure 1. Often times, circadian dysfunctions may occur during the process of ‘entrainment’ or tuning of the internal body clock with external environmental cues causing desynchronization of the clock resulting in onset of what we commonly refer to as neurological sleep disorders [3].
Sleep disorders may be caused by physical or mental conditions, genetics, side effects of ailments, medication, lifestyle factors, hormonal changes, ageing, environmental factors, etc. There are different types of sleep disorders that are categorized as dyssomnias or parasomnias which are further segregated into far more complicated subdivision of myriads of disorders [1]. Circadian rhythm sleep disorders include delayed sleep-wake phase disorder (DSWPD), advanced sleep wake phase disorder (ASWPD), irregular sleep-wake rhythm phase disorder (ISWRPD), Jet-lag disorder, Shift-work disorder, etc. [2]. This article succinctly covers four commonly known sleep disorders shown in Figure 2. Sleep is directly influenced by one extrinsic factor, one of which is bedding or sleep surface [4]. Since the mattress is directly relational to sleep as a surface, it has been proven scientifically that modulating sleep surfaces does help rehabilitate individuals with improved sleep latency (the time it takes to fall asleep), sleep efficiency (percentage of time spent in deep sleep) and total sleep cycle duration (to ensure fully energized wake cycles) [5].
Methods
Innovations in material science influencing sleep
Innovative surfaces play a role in ‘sleep medicine’ whereby they can either complement medication for sleep disorders or even minimize dependence on medication as the only remediation [4]. I believe we need far more comprehensive information to enable people to make informed choices on how to customize sleep surfaces and sleep environments to overcome sleep disorders. Majority of people are not aware of the significance of the composition of sleep surfaces. There has been significant evolution in the role of mattresses, their composition, architecture and associated bases which may be static or active. This isn’t just a comfy-vs-uneasy or tossing-vs-tranquil debate but a far more intricate issue where each material has the capacity to influence the quality of sleep [6]. This article provides a foundational basis to understand how different types of materials in mattresses can maximize potential for overcoming sleep impairment. We need to explore the specific ways in which bedding materials in the retail industry impact sleep disorders to emphasize the important connection between our sleep setting and our overall health [4].
It is also necessary to appreciate that developments in material science and sleep systems have benefited lifestyles worldwide to produce and manufacture a fascinating range of mattresses and associated accessories such as sheets, pillows, duvets, toppers, adjustable bases, etc. [7]. These directly impact sleep architecture which is normal succession of sleep stages during a night’s sleep [6]. Culturally different ethnic-communities have preferences for using different kinds of sleep surfaces that enhance their sleep patterns [8]. Few prefer firm surfaces others medium and others plush with different materials. There is no one size, or one make that fits all. Each person or couple is unique; based on his/her body mass index (BMI) they need different pressure zones for enhancing sleep in a sleeping posture [9]. Wrong selections do not allow them to sleep properly at all. Factors like the firmness of mattress, types of springs, and the support of pillows, thermoregulation, and the very makeup of regular bedding can all influence sleep patterns across different age groups or ethnicities strongly. The right bedding can also combat sleep disturbances caused by hypersensitive skin reactions or dust/allergies [10]. Hypoallergenic materials like bamboo and microfiber resist common allergens like dust mites and mould [11]. Several sleep-systems including adjustable bases, smart mattress and AI mattresses have the capacity to enhance sleep health in people and societies [12].
Results
Prevalence of sleep disorders in New Zealand
Previous research studies have indicated the significant burden of sleep problems in different age groups particularly adults in New Zealand in 2019 and 2022. Prevalence estimates for insufficient sleep in the 2019 New Zealand Health Survey were derived using complex survey weighting and age‑standardisation, consistent with the standard NZHS methodology; group differences in published NZHS‑based sleep analyses have typically been assessed using design‑based chi‑square tests and multivariable logistic regression models [13].
Insomnias: Currently, 25% of adults have chronic sleep problems in New Zealand, with insomnia as the most common sleep disorder [14]. Insomnia grew significantly from 13% in 2001 to appx 25% in 2025 in New Zealand [15]. Thus, as a public health issue, it affects approximately one in four adults in New Zealand due to a combination of lifestyle (e.g. addictions), environmental (e.g. lack of exposure to adequate sunlight), psychological (e.g. stress), and systemic health factors (e.g. ailments or ageing) [15].
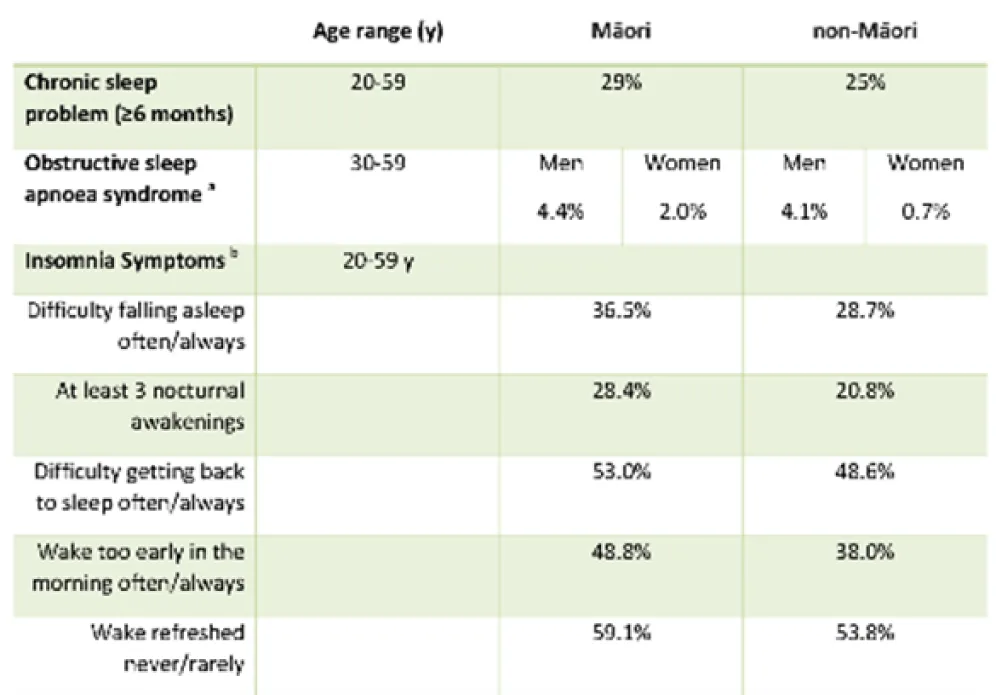
Obstructive Sleep Apnea (OSA): About 3% of adults have OSA, but prevalence varies by gender and ethnic background; showing that Maori men are more likely to have it than non-Maori men or general multi-ethnic population of women [16]; seen in Figure 3. Demonstrating that Māori and Pacific people have higher prevalence of short sleep and sleep‑disordered breathing symptoms than European/Other groups.
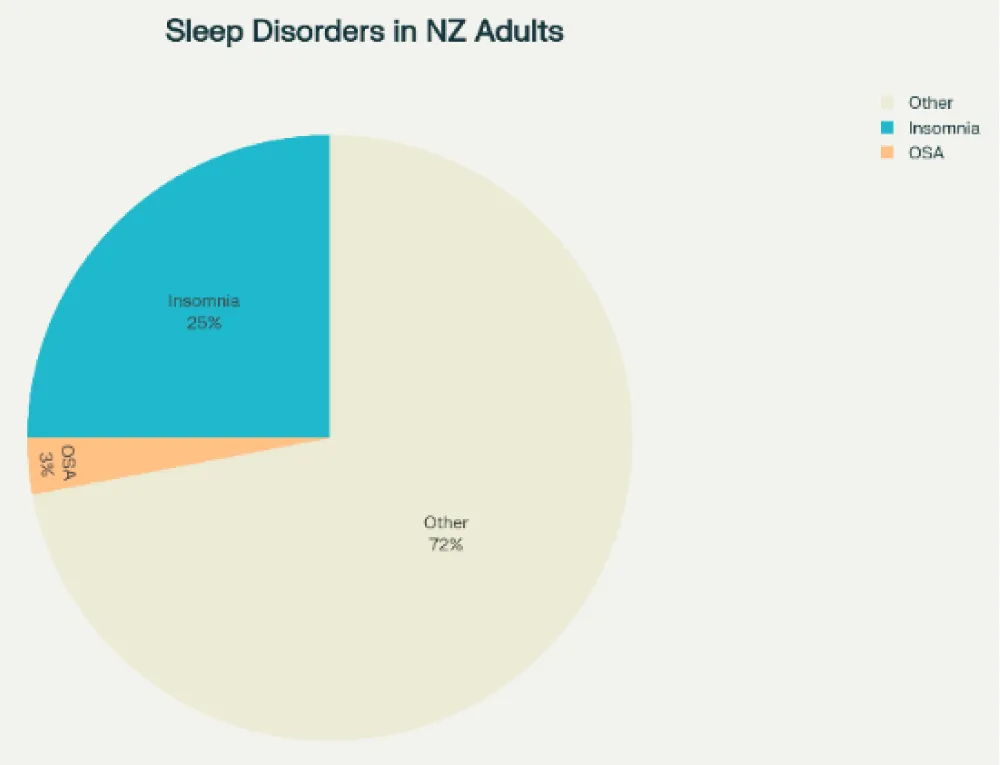
Other or unspecified sleep disorders: The rest of the problems cover a broad-spectrum range of circadian disorders including parasomnias, less common sleep-related breathing or movement disorders [17]. The following color pie chart (Figure 4) depicts common different sleep disorders among adults in New Zealand, based on the most recent data-surveys over the past two decades by Government agencies (fairly large sample sizes were used), with women consistently showing higher prevalence of poor sleep quality than men across age groups.
Discussion
Correlating sleep disorders and restorative therapeutic surfaces
Given that New Zealand’s total population averages approximately 5.2 million (2023 Census), with roughly 50.3% female and 49.3% male; about 16% of the population is aged 65 and over with 17.5% identifying as Māori. The fact that 25% of adults equating to about 1.3 million individuals suffer from chronic sleep problems underscores the substantial public health burden. Notably, this prevalence affects diverse demographic groups, including Māori communities, who often experience disparities in sleep health outcomes [13,18]. This highlights the critical need for targeted interventions, such as the development of restorative-therapeutic sleep surfaces, to address this pervasive issue across the population. Quality of sleep has been shown to improve with high-quality bedding [5]. Thereby necessitating targeted rehabilitation techniques, one of which is modulating sleep surfaces. This discussion elucidates how bedding choices, customized sleeping surfaces and sleep systems can improve common sleeping disorders.
Insomnia, defined as having difficulty falling asleep, maintaining sleep, or obtaining restorative sleep, is a common problem that affects millions of people world-wide. Although there are many causes of insomnia which are multi-faceted and may include psychological, physiological, or environmental influences, it is now evident that silk bedding can have a positive impact over other materials [9]. Moreover, a mattress that is too firm can cause uneven pressure points and frequent wakings. On the flipside, if a mattress is too soft there may be lack of support, causing improper alignment of the spine and thus producing back and joint pain, making sleeping difficult [19].
Insomnia is usually best treated using a mattress that is a medium firm, custom made to order, ensuring ergonomic zoning in the mattress to ease surface tension corresponding to the body’s main pressure points [9]. The five key pressure points while on a sleeping surface are the head, shoulders, hips, knees and ankles. Currently in New Zealand, there are mattresses which may be designed as unzoned or subdivided into three zones, five-zones or seven-zones. The five-zone mattresses are quite effective and suitable for adults and couples. However, a high ergonomic mattress providing the seven-zone pressure relief system could work best for people suffering from insomnia or neurological or orthopedic ailments [20]. A hybrid mattress combing memory foam and latex is generally most effective with zones packed with high tensile pocket springs [9]. A corresponding medium sized pillow will work better to align the spinal posture adequately to induce sleep quicker. Costings of different manufacturers and suppliers vary, however, invariably investment in high quality therapeutic surfaces has known to improve health sustainably over the long term [21].
Few studies have examined the evidence for the efficacy of special mattresses and bedding including an adjustable base for the treatment of insomnia and chronic snoring. The elevation provided by an adjustable remote-controlled base elevates the upper half of the body to ease breathing through constricted nasal cavities or trachea to improve airflow and expand lung capacity [12]. The zero-gravity (Zero G) position induced by the adjustable bases enhance better blood circulation [21]. Earlier study showed that Temperature-controlled sleep systems can improve subjective sleep quality and thermal comfort [22]. Moreover, earlier studies showed how temperature-regulating mattresses improve sleep quality [4,7]. This emphasizes the need for a comfortable sleep temperature that is cooler. These findings emphasize the importance of personalized sleep systems according to body weight, sleep position, and thermoregulatory preferences.
Sleep Apnea is another common sleep disorder that has impacted overall health. Sleep apnea is characterized by repeated interruptions of regular breathing throughout the night that causes snoring, gasping, choking, pauses during breathing, frequent awakenings and groggy feeling during the day. Though the commonly used therapy for sleep apnea is continuous positive airway pressure (CPAP), associated bedding may be a complementary component to help enhance sleep quality and treatment of chronic symptoms. The most direct impact comes through positional therapy using mattresses, pillows, or devices that help keep a person sleeping on their side, rather than their back [23,24]. These are medium to soft mattresses that readily compress on the shoulders and hip regions. Sleeping on the back can worsen obstructive sleep apnea (OSA) because the tongue and soft tissues may collapse backward and block the airway. Side-sleeping helps keep the airway more open and reduces apnea events for most people. Hence a mattress which encourages uniform rather undulating alignment of the spine can help to open the airway and can minimize the severity of apneic episodes. Undulating mattresses that are overly soft, by contrast, could worsen sleep apnea by allowing the neck to flex too much, narrowing the airway.
People with sleep apnea typically do well with a double spring mattress that provides customized support and pressure relief, especially for those with high body mass index (BMI). Temperature regulation is essential for sleep apnea. Too much insulation can exacerbate sleep apnea due to overheating, hence pure (natural) latex is generally considered better than synthetic latex. Natural latex offers superior breathability and hypoallergenic properties compared to synthetic latex, making it a more comfortable choice for individuals with sleep apnea [24]. Cooling gel layers or gel-infused foams may be better as a thermoregulating surface to lower the body temperature. A breathable fabric is better than a synthetic fabric or polymer. Breathable, natural fabrics like cotton, linen, and bamboo can help regulate body temperature and promote better airflow, which is particularly helpful for conditions like sleep apnea [7]. Additionally, weighted blankets have shown promise in reducing anxiety and improving sleep for some individuals.
Narcolepsy is another chronic neurological sleep disorder. Symptoms include sleepiness and a propensity to abruptly fall asleep during inappropriate day hours. This results from the brain’s inability to appropriately define fixed sleep-wake cycles. Other symptoms of narcolepsy include hypnagogic hallucinations (strong dreamlike experiences during sleep or wakefulness), sleep paralysis (temporary incapacity to move or speak during sleep or wakefulness), and cataplexy (sudden muscle weakness brought on by strong emotions). The actual cause usually is loss of neurons in the brain that produce hypocretin, also referred to as orexin, which aids in regulating wakefulness, is frequently the precise cause. Medication, lifestyle changes, and sleep patterns can all help control symptoms. For narcolepsy, pressure-relieving surfaces that accommodate multiple sleep positions support the irregular sleep-wake patterns characteristic of this disorder [20]. The effects of specialised mattress toppers or an inbuilt topper with pressure-relieving memory foam or latex mattresses with spinal alignment support need to be studied in this regard. Moreover, temperature regulation technology helps reduce discomfort, minimize disturbances, and promote deeper sleep cycles at night [14].
Restless legs syndrome (RLS) is a neurological condition involving an uncontrollable urge to move the legs, often with an unpleasant sensation. The symptoms of RLS tend to aggravate when at rest or not doing any activity and can have a marked effect on sleep. There’s no one bedding product that will cure a case of RLS, but the right array of bedding can alleviate its symptoms and improve sleep. If a mattress is supportive and relieves the pressure off the lower back, there is less discomfort and kicking of the legs. When the spine remains in proper alignment, tension and pain in one’s legs can be reduced, and, in turn, the frequency of RLS symptoms can be reduced [10]. A high-profile pillow can provide the necessary support to one’s neck and head that may result in a state of complete relaxation. The temperature of the bedding is also key; RLS sufferers often prefer a cooler bed to reduce symptoms. So, cotton sheets and light blankets are most suitable. In addition, certain bedding can cause RLS symptoms to worsen in some people. For example, some people experience increased RLS symptoms when using artificial or chemically based bed linen. Opting for natural, hypoallergenic sources of bedding can be advantageous in minimizing irritants and upgrades the quality of sleep [11]. Regularly washing sheets is crucial to help rid the bed of potential allergens that can exacerbate RLS symptoms.
Conclusion
In summary, there is a definite link between bedding and sleep-related issues. Direct intervention using appropriate therapeutic sleep surfaces has been shown to improve sleep quality in individuals with sleep disturbances [5,9]. Rehabilitation is possible to complement and supplement treatments for sleep disorders using appropriate therapeutic mattresses, pillows and bedding elements that alleviate symptoms and improve sleep quality in insomnia and related conditions [5,9]. This same fact possibly even applies to parasomnias, or unusual actions and physiological events that occur while a person is asleep. For instance, mattresses or pillows contributing to frequent nighttime arousals could theoretically heighten sleepwalking risk in predisposed individuals. On the other hand, a relaxing sleep environment that minimizes arousals could reduce parasomnia occurrence. It is also important to identify and debunk bedding myths. One of these is that a ‘firmer mattress is a better one’. That is analogous to overuse of the ‘harder is better’ fallacy which may not be suitable for certain sleep conditions [19]. Firmness is crucial, but the perfect amount of firmness can differ a lot depending on personal factors such as body mass index, favourite sleeping position, and existing health issues. Drake, et al. [25] supports the personalization principle by documenting how sleep perception mismatches in insomnia patients mean subjective comfort (influenced by BMI, position, health) must guide firmness selection over rigid rules. Another myth is to sleep “in” snugly rather than “on” the surface. This compares two contrasting ends of the spectrum. A mattress that’s too soft and lacks support will fail to support the spine in proper alignment, will strain and put pressure on joints, and may even aggravate OSA and cause musculoskeletal problems [19]. Well-made hybrid mattresses accommodate the curves of the body compress adequately, without creating uneven tension points [20]. Another source of confusion is “one type of bed or foam type is best for all health problems” this again may not be entirely accurate. Given the disparities in sleep health among different ethnic groups in New Zealand, targeted interventions that consider cultural and physiological differences are essential for effective management [8,16]. Recently, integrating AI-Sleep Systems tailored to individual needs is shown to hold significant potential to restore sleep health and reduce the burden of sleep dysfunctions and associated neurological disorders across New Zealand [26] which can negatively affect mental health and wellbeing of the public [27].
References
- Czeisler CA, Gooley JJ. Sleep and circadian rhythms in humans. Cold Spring Harb Symp Quant Biol. 2007;72:579-597. Available from: https://doi.org/10.1101/sqb.2007.72.064
- Moore RY, Eichler VB. Loss of a circadian adrenal corticosterone rhythm following suprachiasmatic lesions in the rat. Brain Res. 1972;42(1):201-206. Available from: https://doi.org/10.1016/0006-8993(72)90054-6
- Mistlberger RE, Skene DJ. Social influences on mammalian circadian rhythms: Animal and human studies. Biol Rev. 2005;80(3):465-480.
- Krystal AD, Edinger JD. Measuring sleep quality. Sleep Med. 2008;9(Suppl 1):S10-S17. Available from: https://doi.org/10.1016/s1389-9457(08)70011-x
- Bertisch SM, Wells RE, Smith MT, McCambridge MA. The role of the bedding environment in sleep quality: A systematic review. Sleep Med Rev. 2014;18(1):87-94.
- Krauchi K, Cajochen C, Mori D, Graw P, Wirz-Justice A. Warm feet promote the rapid onset of sleep. Nature. 1999;401(6748):36-37. Available from: https://doi.org/10.1038/43366
- Okamoto-Mizuno K, Mizuno K. Effects of thermal environment on sleep and circadian rhythm. J Physiol Anthropol. 2012;31(1):14. Available from: https://doi.org/10.1186/1880-6805-31-14
- Paine SJ, Harris R, Gander PH, Reid P. Prevalence and consequences of insomnia in New Zealand: Disparity between Māori and non-Māori. Aust N Z J Public Health. 2005;29(1):22-28. Available from: https://doi.org/10.1111/j.1467-842x.2005.tb00743.x
- Jacobson BH, Boolani A, Smith DB. Changes in back pain, sleep quality, and perceived stress after introduction of new bedding systems. J Chiropr Med. 2009;8(1):1-8. Available from: https://doi.org/10.1016/j.jcm.2008.09.002
- Trenkwalder C, Winkelmann J, Inoue Y, Paulus W, Oertel WH. Restless legs syndrome—current therapies and latest advances. Nat Rev Neurol. 2016;12(8):434-445. Available from: https://doi.org/10.1038/nrneurol.2015.122
- Allen RP, Picchietti D, Hening WA, Trenkwalder C, Walters AS, Montplaisir J. Restless legs syndrome: Diagnostic criteria, special considerations, and epidemiology. Sleep Med. 2003;4(2):101-119. Available from: https://doi.org/10.1016/s1389-9457(03)00010-8
- Thorpy MJ, Yager J. Sleep disorders and sleep deprivation: An unmet public health problem. Sleep. 2011;34(5):555-556.
- Ministry of Health NZ. Annual Data Explorer 2019/20: New Zealand Health Survey: Insufficient Sleep. 2019. Available from: https://www.health.govt.nz/publications/annual-update-of-key-results-201920-new-zealand-health-survey
- Paine SJ, Smith C, Gander PH. Insomnia prevalence and consequences in New Zealand: Disparity between Māori and non-Māori. Aust N Z J Public Health. 2018;42(6):590-596.
- Paine SJ, Gander PH, Harris RB, Reid P. Prevalence and consequences of insomnia in New Zealand: Disparities between Māori and non-Māori. Aust N Z J Public Health. 2004;28(2):116-125. Available from: https://doi.org/10.1111/j.1467-842x.2005.tb00743.x
- Brabyn S, Cormack D, Smith C, Gander P. Obstructive sleep apnea in New Zealand adults: Prevalence and ethnic differences. Sleep Health. 2022;8(1):1-8.
- Ancoli-Israel S, Kripke DF, Klauber MR, Mason WJ, Fell R, Kaplan O. Sleep-disordered breathing in community-dwelling elderly. Sleep. 1995;18(4):291-298.
- Stats NZ. 2023 Census: Population counts. 2023.
- Kovacs FM, Abraira V, Peña E, Martín E, Sánchez A, Muriel A, Gómez JL, Gil del Real MT. Effect of firmness of mattress on chronic nonspecific low-back pain: Randomized, double-blind, controlled, multicenter trial. Lancet. 2003;362(9396):1599-1604.
- Radwan A, Fess P, James D, Johnson A, Mills C, Murphy VS. Effect of different mattress designs on promoting sleep quality, pain reduction, and spinal alignment in adults with or without back pain: Systematic review of controlled trials. Ergonomics. 2015;58(1):23-41. Available from: https://doi.org/10.1016/j.sleh.2015.08.001
- Park KE, Choi JH, Lee SH. The impact of adjustable/zero-gravity beds on upper airway patency for obstructive sleep apnea. Sleep Breath. 2017;21(3):537-543.
- Lee HY, Kim JH, Park SY. A preliminary study of the effect of mattress temperature regulation on sleep quality. Chronobiol Med. 2022;4(2):49-55.
- Oksenberg A, Silverberg DS, Arons E, Radwan H. Positional therapy for obstructive sleep apnea syndrome: A therapeutic effect of sleep position. Sleep. 2000;23(6):745-751.
- Jones SE. Bedding materials for adult sleep apnea: A systematic review. Nat Sci Sleep. 2021;13:2035-2045.
- Drake CL, Pillai V, Roth T. The subjective-objective mismatch in sleep perception among those with insomnia and sleep state misperception: Implications for bedding choices. Sleep Med Rev. 2017;33:36-43.
- Satralkar M. Advancing AI-Sleep Systems to restore Neurological Sleep Disorders and Precision Health in New Zealand. J Neurosci Neurol Disord. 2026. In press.
- Ludin N. Mental Health and Sleep Disorders. Auckland University Online Publication. 2023.


 Save to Mendeley
Save to Mendeley

